
Ulcerative Colitis - Kids & Teens
Treatment plan for
Ulcerative Colitis
Medications for Ulcerative Colitis
Mild
disease is more often than not treated with appropriate medications
- surgery is usually reserved for more severe cases, or if
complications arise. If you are not needing to have surgery, don't
worry about the section talking about the different types of
surgery, meeting with the surgeon, and the questionnaire.
In addition to
liquid diets, there are also medicines that may help. Here is a
general list of currently available treatments for ulcerative
colitis in children, including how they work and when they might be
used.
5-ASAs (5-aminosalicylic acid)
This medicine may
be used to help reduce inflammation. It is usually used for mild to
moderate symptoms. It is useful to help lessen symptoms and restore
health (induction of remission), but is not useful for keeping your
symptoms from returning (maintaining remission). It may take 4-8
weeks before you start to feel better.
5-ASAs are usually
taken daily, either orally or rectally (as an enema or suppository).
They are considered a safe treatment option when used long-term.
Examples of 5-ASAs
include: mesalamine, balsalazide, olsalazine and sulfasalazine.
Corticosteroids
Corticosteroids are also used to help reduce inflammation. They help
lessen symptoms and restore health (induction of remission) in
moderate and severe ulcerative colitis. They are not, however, meant
to be used long-term due to side effects.
Corticosteroids may
start relieving symptoms within 1-3 weeks. Remission (having no
symptoms) may be reached within 6-8 weeks.
Usually your doctor
will want to see you again in 2-3 weeks after you have started
taking corticosteroids, to see how you are doing and whether you are
getting good results from the medicine or if you are still having
any problems.
Corticosteroids are
taken by an intravenous tube, orally or rectally (eg, an enema). The
most commonly reported side effect is infection. Other related
problems include bone mineral loss (which may be treated with
supplements of calcium and vitamin D), slowing of growth in
children, increased appetite, weight gain, disturbed sleep pattern,
a so-called 'moon-shaped face' due to fluid retention in the skin
(called Cushing's syndrome), or acne.
For disease at the
end of the small intestine, or right side of the colon, budesonide
(a glucocorticosteroid drug) may be used and is considered to have
fewer safety concerns.
Examples of
corticosteroids include: prednisone, methyl prednisolone (taken by
mouth) and triamcinolone or budesonide (taken rectally).
Immunosuppressants
Two-thirds of people with IBD (Crohn's disease and ulcerative
colitis) will take an immunosuppressant at some point. This medicine
helps keep down inflammation by lowering the activity of the immune
system.
Immunosuppressants
are most helpful for keeping symptoms from returning (maintenance of
remission) and are 'steroid-sparing', meaning they can help reduce
the dose of corticosteroids needed. They are often used to treat
moderate to severe Crohn's disease.
Immunosuppressants take a while to start working (approximately 2-4
months), so they are often taken along with corticosteroids. They
are taken orally (by mouth) for ulcerative colitis.
It is important to
keep taking your medication, as there are good benefits. However,
some people may have to stop because of side effects. It is
important to discuss this with your doctor first. Side effects may
include: nausea, myelosuppression (lowering the bone marrow's
ability to make blood cells, which can require frequent blood tests)
or risk of infection such as viral herpes (eg, cold sores). They
also have a risk of pancreatitis (inflammation of the pancreas).
Treatment with azathioprine or 6-mercaptopurine may also bring about
a slight increased risk of lymphoma (cancer of the lymphatic
system). Regular monitoring, therefore, is important.
If you have any of
these problems, or any other symptoms while taking this medicine,
contact your doctor right away. Your doctor will also probably want
to monitor you regularly while you are taking this medicine.
Examples include
azathioprine or 6-mercaptopurine, also known as 6-MP.
Anti-TNFα
Anti-TNF drugs may be used for ulcerative colitis when other
treatments have not worked well. They work quickly (generally within
2-4 weeks) and are shown to be most helpful in people with
inflammation only in the gut wall.
Currently available
anti-TNFs for ulcerative colitis are given in the hospital
(intravenously through a drip) or at home (by injection).
Before taking this
medicine, your doctor will ask to check you for tuberculosis with a
chest X-ray and/or skin test. There is a risk of infection, although
it is lower than that associated with steroid use. There may also be
an allergic reaction causing joint pain, rash, or a short-term
(transient) reaction or fever. Other potential problems include
heart failure in the elderly (watch for swollen ankles or shortness
of breath) or skin problems.
If you are taking
anti-TNF medicine and have any symptoms such as night sweats, cough
or shortness of breath, contact your doctor.
There have been
rare reports of cancers associated with biological therapy, but it
is not yet known whether these were due to these medicines or to
other medicine given at the same time. Research is ongoing to look
at both possibilities.
An example of an
anti-TNF (in Europe): Infliximab
Medical devices
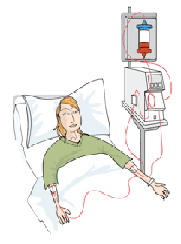 Apheresis
(leukocytapheresis) Apheresis
(leukocytapheresis)
Cells of the immune
system called white blood cells (or leukocytes) defend the body
against infections. In people with active IBD types of leukocytes
called granulocytes and monocytes are often increased or over
active. Large numbers of these cells enter the wall of the
intestines and can release substances that cause bowel injury and
stimulate inflammation. It is believed that the watery diarrhoea
seen in severe IBD is a result of injury to the absorptive
epithelium which makes it unable to absorb water.
Apheresis, or
leukocytapheresis, is performed with a medical device that
selectively binds excess or activated granulocytes and monocytes
from the blood. Blood is pumped from a vein in one arm (via a simple
venopuncture) through a column containing cellulose acetate beads or
a filter. This binds granulocytes and monocytes while the rest of
the blood passes right through and is infused back into the body
through the other arm. The outcome is a reduction in the number of
inflammatory cells that can move from the blood into the intestinal
wall. As a result, the symptoms of IBD are relieved, and the bowel
gets a chance to heal.
The treatment lasts
for 1 hour and is usually given once a week for 5 weeks. It can be
performed in hospital or in an outpatient setting.
Leukocytapheresis involves mainly adults with IBD - there is some debate as to
whether it is suitable for children. It can be used to reduce
symptoms during a severe flare up, or in moderate to severe active IBD in which satisfactory effects have not been achieved with
corticosteroids or other immunosuppressive therapy.
Some temporary side
effects can occur, such as low blood pressure, palpitations, and hot
flushes; however, little is known about the long-term side effects
of apheresis.
The biological
processes through which leukocytapheresis affects the course of
disease remain largely unknown, and it is difficult to draw
conclusions from the existing clinical trial data on how effective
the treatment really is.
| 


